Dr Bot wields the scalpel
-
- from Shaastra :: vol 05 issue 03 :: Mar 2026

Robots are rewriting the rules of surgery, with a precision that humans may find hard to match. A glimpse of the revolution in the operation theatre.
The discussion on robotic telesurgery was in full swing when Indore-based bariatric surgeon Mohit Bhandari, to the surprise of the media he was addressing, suddenly excused himself from the room. The 45-year-old surgeon was back after half an hour. "Sorry, I had to perform a surgery," he said with a grin and the nonchalance of someone who had gone to attend to a phone call.
Bhandari's patient was in Indore, but he went only as far as a room on the upper floor at the head office of SS Innovations International, a Gurugram-based medical technology company that had — on December 23, 2025 — organised what it called a 'telesurgery marathon', and a press briefing on its sidelines. The room where Bhandari had conducted the surgery did not reek of disinfectants. No one was in scrubs; Bhandari, for one, was in track pants, a hoodie and sneakers. The surgeons sat at consoles. Using the instruments before them, they remotely controlled the movements of the company's surgical robot that was performing the operation.
SS Innovations was set up by cardiac surgeon Sudhir Srivastava, who had returned to India from the U.S. in 2011, seeking to advance robotic surgery in his country of birth. His move to India coincided with the end of the first decade of robot-assisted telesurgery. The first such surgery was in 2001, in what is called the Lindbergh Operation, when French surgeons in New York removed a gallbladder from a patient in Strasbourg, France, using a robot called Zeus made by the U.S company Computer Motion. In 2003, Computer Motion merged with the Stanford start-up Intuitive Surgical, the makers of the da Vinci Surgical System, a computer-controlled robotic platform. While robotic surgery grew rapidly, telesurgery did not take off then, due to high costs and issues of connectivity. The All India Institute of Medical Sciences (AIIMS) had bought a da Vinci robot in 2006.
When Srivastava moved to India, the country was importing refurbished robots with only five years' service support from the parent company. Srivastava felt he had to make an Indian surgical robot at a substantially lower cost. "I first tied up with some German engineers. It did not work out," he recalls. Realising that India had the engineering and medical talent, he started all over again in 2017. By February 2021, despite the pandemic slowdown, he was ready to showcase SSI Mantra, a "multi-operation assistant", or a robot that could be used for different types of surgeries. It had performed 18 surgeries across disciplines during the clinical trial stage. Priced at ₹5-7 crore, one-third of the cost of an imported refurbished system, the Mantra consoles quickly reached several Tier II and III towns. Now, over 160 systems are installed across India, including in government hospitals. It has also been exported to Nepal, the Philippines, Oman, Colombia and other countries.
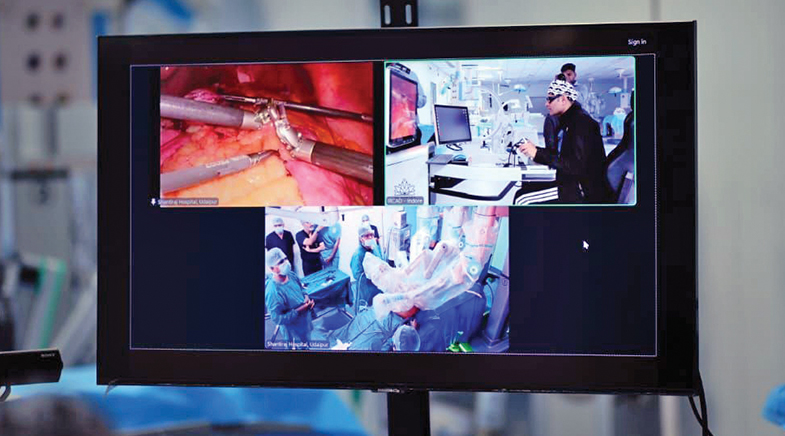
A SURGICAL REVOLUTION
Robots are rewriting the rules of surgery, with a precision that human beings have found hard to match. They bring the power of modern surgery to patients living in smaller cities, while helping surgeons perform complicated operations with confidence. The robot is only one of the features of current surgical practice. Several other technologies are combining to reimagine and recreate the modern operation theatre. Augmented Reality (AR) enhances views of the surgical site. Artificial Intelligence (AI) enables smart theatres that communicate with surgeons. Automated devices stitch up cuts on their own. Nano-robotic surgeons reach where no human scalpel has ever gone before. Techniques are being developed to avoid surgery altogether, in the conventional sense. With these techniques, patients experience less pain, shorter hospital stays, and faster recoveries.
The open console design of the SSI Mantra robot, for instance, provides 3D vision for the entire surgical team, as opposed to the prevailing close-console architecture, which restricts the surgeon's vision. Wireless technology for hand controls offers more freedom of movement than prevailing electromechanical systems. More significantly, it comes with a modular design with three-, four-, and five-arm options that can be removed when not needed, providing greater flexibility than existing products. The fifth equips it for cardiac surgery. Srivastava says that he can conduct a complex quadruple bypass operation using the device on a beating heart.
According to MarketsandMarkets, a market research company headquartered in Pune, the global surgical robot market was valued at $13.69 billion in 2025. It is expected to reach $27.14 billion by 2030. Roughly 65% of this market is in North America, which also hosts the world's leading robotic manufacturers, including Intuitive Surgical, Medtronic, and Johnson & Johnson. China is the fastest-growing market, and several Asian countries — including India — are expanding their robotic surgery infrastructure. According to a January 2026 statement from Intuitive Surgical, da Vinci has been used in 20 million surgeries so far, for a wide variety of procedures, including several thousand mitral repairs in the heart.
SHRINKING DISTANCE
In July 2000, when Intuitive Surgical got clearance from the U.S. Food and Drug Administration for clinical use of the da Vinci robot, it was deemed equivalent to laparoscopic equipment in terms of safety. So, the initial clearance was for minimally invasive abdominal procedures. It forged ahead of laparoscopy in capabilities over the next two decades. The robot was cleared for different procedures, including urologic and prostate surgeries. In the past decade, it has been cleared for cardiac, colorectal, gynaecologic and other such surgeries. While laparoscopy offers cost and ease-of-use advantages and is expected to remain in use for at least another decade or two, robots introduced a new path for surgical advancement.
One of the advances that robots brought was in the way the surgical arm could be manoeuvred. A laparoscopic surgeon could move the instrument in and out of the body, tilt it left or right, tilt it up or down, and rotate it along one axis. The robot arm could move or rotate in all three directions. It had another advantage: the arm tip could be moved like a human wrist. The robotic wrist enabled fine manoeuvres within the body, which, in turn, improved reconstruction and suturing during surgery, among other things. Moreover, the robotic arm eliminated the tremor of normal human hands. In other words, digital motor control reduced the impact of human frailties.
Similarly, robots used advanced imaging technologies to improve the depth of vision, introducing three-dimensional optics and magnification using stable cameras. Overcoming the limitations of the human eye and brain was just as important for surgery as mechanical freedom and precision. These two advances, along with good architecture, control algorithms, and standardised platforms, spread the use of robotic surgery in the developed world.
Significant improvements in communication also enabled telesurgery with the use of robotics. The aim of the robotics companies, however, was not telesurgery. It was to introduce precision to surgical procedures. But India had different market needs.
Personalised surgical planning using digital aids is now increasingly common across areas such as neurosurgery, dentistry, orthopaedics, and reconstructive surgery.
The Indian healthcare system is dominated by large cities and a few hospital chains. According to the Indian Hospital Market Outlook to 2030 report (bit.ly/hospital-outlook) by Ken Research, a market research company, India had a shortage of 600,000 doctors and two million nurses in 2023, with only one doctor available for every 5,000 patients in rural areas. Not surprisingly, there is considerable hope in the country about the reach of the robotic arm.
Since July 2025, when Srivastava showcased the capability to perform a cardiac procedure on a patient in India while attending the annual conference of the Society of Robotic Surgery at Strasbourg, France, over 100 operations have been conducted on Mantra consoles. These include some complicated procedures. For example, urologist V. Chandra Mohan, Managing Director of Preeti Kidney Hospitals, Hyderabad, performed pyeloplasty from Gurugram on a 16-month-old patient in Hyderabad. The surgery was to remove a congenital blockage that prevented the flow of urine from the kidney to the ureter.
In December 2025, Mumbai's Kokilaben Dhirubhai Ambani Hospital & Medical Research Institute conducted two cancer surgeries with the surgeon sitting some 5,000 km away in Shanghai, with the Toumai Surgical Robot. Priced at ₹7-13 crore, the Toumai is made by the Chinese company MedBot Surgical, which is increasing its presence in India. "During complications in a surgery, it will become easier for an expert to join in remotely than for us to wait for them to reach the hospital, scrub up and join," says Bhandari.
According to the surgeon, the full impact of telesurgery will become apparent over the next few years, as more robots enter the market. "India has such a huge need for surgical aid to reach the last mile that no single player can reach out to all,” says Sudhir Rawal, genito-urinary oncology surgeon at the Rajiv Gandhi Cancer Institute and Research Centre, Delhi. "Even if ten companies enter the fray, we will not be able to meet the demand," says Rawal, who was associated with validating SS Innovations's telesurgery systems.
Telesurgery has been enabled by advances across diverse fields. First, the improvement in communications. A telesurgery system can tolerate delays of only 150 milliseconds, beyond which the surgeon begins to feel a lag and loses fine control. The reliability of communication has been demonstrated in special situations. SS Innovations uses a dedicated fibre network and supposedly has delays of only 50 milliseconds. Toumai has demonstrated telesurgeries over 5,000 km using satellite link-ups between Lhasa and Beijing, with delays within acceptable limits. In addition to optical fibre links, the past two decades have seen the development of real-time operating systems, rapid conversion from analogue to digital and back, video compression technologies and embedded processors — all of which have enabled telesurgery.
However, despite the demonstrated success of telesurgery, medical technologists feel that, for it to become widely used around the world, several improvements are needed at the system level. These include improvements in haptic feedback, redundancy at multiple levels to ensure a fail-safe system, data protection, and standardisation of legal frameworks.

SMART OPERATION THEATRES
Subhamoy Mandal, Assistant Professor at the School of Medical Science and Technology at the Indian Institute of Technology (IIT) Kharagpur, uses the analogy of cars to explain much of the research on imbuing operation theatres with new technology. At present, surgeons learn about a patient by studying scans — X-rays, MRIs, CTs — before opting for a procedure. During surgery, however, they proceed unguided. With minimally invasive surgeries that are now the norm, the surgeon's view into the patient is restricted through the laparoscopic camera. "Now imagine a GPS-like guided system that takes data from these scans and overlays it on the video screen, providing a roadmap within the body for the surgeon," Mandal says. Such a map would give clear anatomical references, showing the lay of blood vessels, fat, and the tumour. These surgical navigation systems are akin to Advanced Driver Assistance Systems (ADAS) in cars, issuing alerts when an action deviates from the surgeon's intended course. At a more advanced stage of autonomy, perhaps the system could even stop a wrong move, Mandal foresees.
Models on which surgeons train are evolving from doll-like mannequins to mixed-reality simulators that incorporate a range of technologies.
A semi-transparent overlay of images, a digital model superimposed on the live image, can show blood vessels, tumour boundaries, and clear safety margins. But overlaying images onto a live body is an extremely challenging engineering problem. The body on the table is dynamic: it breathes, moves, bleeds, and deforms when touched. Scientists are developing methods to match dynamic body data to images, and they expect varying degrees of success depending on the tissue type. Since the bone is a hard tissue, scientists expect adoption over the next few years. In softer tissues such as the abdomen, image overlays are not likely to happen before 2035, or even take longer. The beating heart makes overlays difficult in cardiac surgery; no one knows how long it will take.
Cartosense, a Bengaluru-based company spun out of IIT Madras in 2017, has an Augmented Reality system for neurosurgery. Its core product is a wide-range camera that receives inputs from infrared emitters in surgical instruments to compute their locations with sub-millimetre accuracy. This live positional information is displayed on a screen and helps the surgeon make important decisions during the operation. Such systems enable the surgeon to avoid critical brain structures and major blood vessels. "Ten years ago, surgeons would say that their experience was good enough for them to operate," says Cartosense founder Nikhil Chandwadkar. "But now that is no longer the case. Their mindset has shifted."
As positional intelligence advances, robots also develop situational awareness, enabling automation. "Many non-critical steps in surgery can be taken over by robotics," says Mandal. Suturing incisions after surgery is one. In India, start-ups such as Denovo Bioinnovations are developing products for auto-suturing and other surgical procedures. A robot conducting an entire surgery, even taking autonomous decisions, might be technologically feasible soon. In 2025, at Johns Hopkins University, a robot trained on gallbladder surgeries performed a surgical procedure on a life-like model, responding to and taking advice from voice commands during the surgery. Named the Soft Robot Transformer-H, it is an advancement on an earlier model developed by the same team under medical robotist Alex Krieger. The previous robot had even performed a surgery on an animal model (bit.ly/robot-surgeon).

Creating a smart operation theatre is another area of research. This involves creating software trained in machine learning that provides situational awareness of the room through cameras, tracks the movement of staff and machinery, monitors equipment condition, and issues alerts. "Such an interactive OT can prevent horrors like missing a step or leaving something behind in the patient's body," notes Mandal, whose team is working in this field.
TWIN TO TANGO
In May 2020, a child from Egypt with a very weak heart that wasn't contracting enough was airlifted to Chennai. The child had suffered multiple cardiac arrests. In addition, there was high blood pressure in his lungs. A heart transplant was not possible for him because the waiting list for a donor was long. The other option was to implant a ventricular pump to help the heart function. For doctors at Chennai's MGM Healthcare, the dilemma was whether the pump, created for an adult, would be fit for the child, and whether it would function well, given that the heart chamber was heavily bound by excess muscle tissue. There was no precedent to rely on, as such a procedure was being attempted for the first time in India.
K.R. Balakrishnan, Chairman of Cardiac Sciences at the hospital, approached his friend, R. Krishna Kumar, now a Professor of Biomedical Engineering at IIT Madras. Krishna Kumar's team built a digital twin, a 3D virtual reality model of the child's anatomy and physiology from his CT scan images. "We donned 3D glasses and worked with the model, practising with different approaches. Based on that knowledge, we could confidently perform the procedure on the child," recalls Balakrishnan. It was among the earliest uses of Virtual Reality (VR) in paediatric cardiosurgery worldwide. The child was discharged after a month. Four years later, he received a transplant.
Personalised surgical planning using digital aids is now increasingly common across areas such as neurosurgery, dentistry, orthopaedics, and reconstructive surgery. However, these systems still lack validation protocols and regulatory pathways. Data privacy and patient consent will be among the issues to be resolved when the technology becomes mature for market launch (bit.ly/Validation-Need). "The use of digital twins in practising, planning and post-operative management of surgeries is poised to take off in a big way in the near future," says Balakrishnan. "At present, though, it is still in its infancy. Only doctors who have access to an institute may be able to use it; there is no software available in the market, yet," he adds.
While bots will not replace the actual surgery to excise a tumour, they will mop up cells that have escaped.
In the future, digital twins that incorporate clinical, imaging, molecular, physiological, and behavioural data and continuously provide the data to the surgeon would be integrated into the next generation of surgical consoles. Krishna Kumar, who believes that digital twins will complement the development of autonomous robotics, is working towards designing such a system. "We already have much of the hardware. Any robot can be programmed to reach a particular path [surgically]. We have to develop the software to create digital twins to plan that path," he explains. Before performing a surgical task, the robot will train on a digital twin of the patient. "Organs like bones or gallbladder are easy to work on; the challenge comes with the heart, which is constantly pumping. But we will get there, soon," he says.
Meanwhile, models on which surgeons train are evolving from doll-like mannequins to mixed-reality simulators that incorporate a range of technologies and novel materials mimicking the complexity of actual tissues. Researchers at IIT Kharagpur, for instance, have developed a mixed-reality simulator, SurgiKLAR, for training in uterine surgery. They continue to work on the model to improve precision and safety, and to extend it to other surgical domains (bit.ly/SurgiKLAR-model).
NANO SURGEONS
Not all regions of the body are easy to access, even with the best instrumentation. Could a tiny specialist be dispatched to that location for the mission? A nanobot or nanorobot is a tiny structure, much smaller than a standard human cell. It can be sent in swarms to ferry payloads to the target destination in the body. While much of the technology for medical nanorobots is still at the proof-of-concept stage, some developments outline the likely direction of progress in the field.
Nanobots could also be deployed for future nanosurgeries to enable biopsies of difficult-to-access body parts.
A research team led by the Shanghai Jiao Tong University School of Medicine published a paper in 2024 detailing success in animal studies using magnetic nanobots to treat a brain aneurysm. Aneurysms are blood-filled bulges in the artery, which, left untreated, can rupture or clot, with life-threatening consequences. The prevalent treatment — long and complex — is for the surgeon to guide a micro catheter to the site to resolve the bleeding and put a stent there. The researchers loaded blood-clotting medication onto the nanobots and coated each with a temperature-sensitive shell. Once the swarm reached the target, an external magnetic field was applied, heating the bots to their melting point and releasing the medication (bit.ly/Clot-Bots).
Using such nanorobots to treat brain disorders and cancer is the aim of Theranautilus, a start-up from the Indian Institute of Science, Bengaluru. Its co-founder, Debayan Dasgupta, notes that cancerous cells are "stickier" or have a higher charge than regular cells. Magnetised nanobots will cling to them more effectively. With an externally applied magnetic field, these bots can be heated to 70-80° C, which is hot enough to kill cancer cells. While the bots will not replace the actual surgery to excise a tumour, they will act as a post-surgical mop-up to catch cancerous cells that have escaped into the bloodstream and are capable of metastasising. Magnetised bots could similarly be used in places in the brain that are difficult to access surgically.
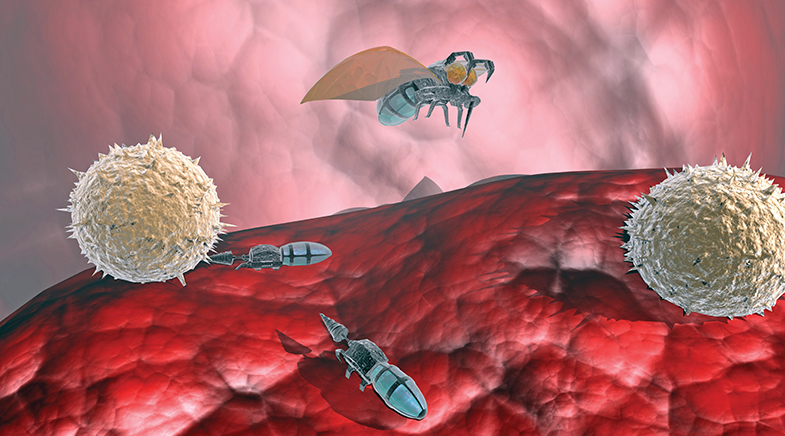
While these technologies are still in early animal trials, Theranautilus has a product for sensitive teeth. Toothpastes for sensitivity form a temporary coating on the dentine where the enamel is eroded. However, they provide only temporary relief. The dentine contains microtubules which reach the sensitive nerves in the tooth pulp. The company has a solution of magnetised dental cement made from nanomaterials, which is magnetically pulled into the microtubules, sealing them and providing permanent relief. The product is at the pre-clinical stage of development.
Nanobots could also be deployed for future nanosurgeries to enable biopsies of difficult-to-access body parts. In 2020, researchers at Johns Hopkins University, U.S., created therapeutic nanobots, which they named theragrippers for their ability to use pincer-like appendages to cling to the inner lining of the gut (bit.ly/theragripper-biopsy). The initial experiment was to demonstrate their ability to deliver drugs with precision, but they could be remodelled to pinch out tissue for biopsy.
"The joystick is still in the hands of the doctor. Only, the tools are evolving," says Dasgupta.
See also:
Have a
story idea?
Tell us.
Do you have a recent research paper or an idea for a science/technology-themed article that you'd like to tell us about?
GET IN TOUCH














